Homecare professions - Operational excellence at the service of people
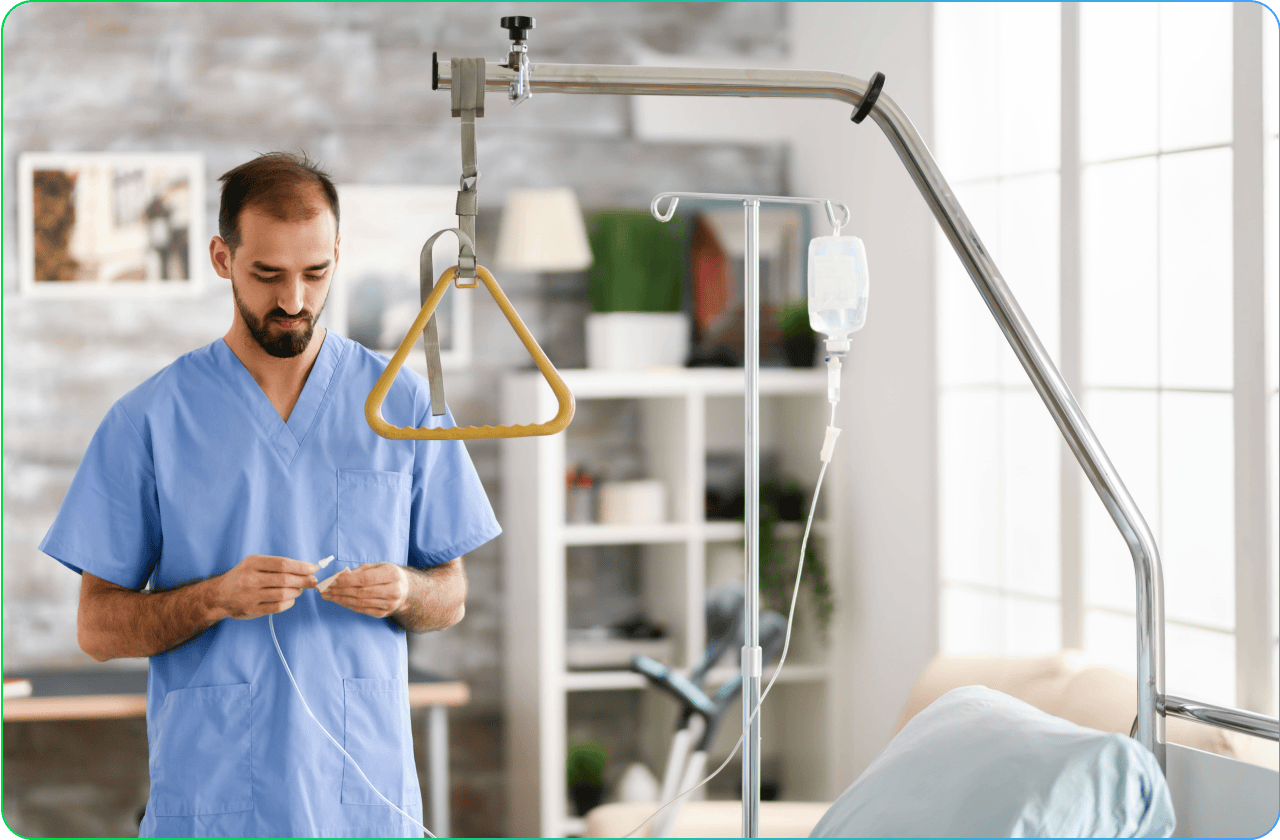
The rapidly expanding home health care (HHC) and home support (HS) professions must meet extremely high standards of quality, punctuality and safety. The daily challenge of these professions is to reconcile these operational requirements with the primary expectation of patients looked after at home: the quality of the human relationship.
Who are the key players in home health?
Of course, when it comes to home care and maintenance, the first thing that comes to mind is the nurses and care assistants who visit patients to take samples, give injections, change dressings, or provide hygiene care that the patients are temporarily or permanently unable to perform themselves. But these health professionals, whose role is obviously central, are far from being the only ones to be involved with patients!
Hospitalisation at home for patients, as well as homecare for the elderly who are losing their independence, would simply not be possible without the technicians who deliver, install and adjust the medical devices they need. These range from medical beds to patient lifts, respiratory assistance systems, and dialysis machines. Whether purchased or rented, all such equipment is subject to strict rules of installation, use and maintenance which it is the responsibility of home health care providers (HHCPs) to respect and enforce.
For this reason, the mission of HHCPs is not limited to the provision of materials and consumables covered by the legislation on medical devices. It covers in particular:
- checking that the devices and their settings comply with the medical prescription, throughout their installation for the patient;
- the control of compatibility between the different devices prescribed to the same patient;
- the management of social security and supplementary health insurance coverage, with all that this implies in terms of confidentiality and security of personal and health data;
- and, crucially, the training of those who are required to use these devices, i.e. the patients themselves when they are sufficiently autonomous to assimilate instructions and perform the required actions, their personal carers (family carers, care assistants) and the professional carers.
It is clear that home health care — and especially its development in response to the ageing of the population and the increase in disabling chronic diseases — is based on the coordination of very different but fundamentally complementary professions, all of which share the common objectives of ensuring the safety, well-being and peace of mind of the patient.
The visit, the keystone of the relationship with the patient
Whether it is for the purpose of care, installation of a medical device, or maintenance, the visit to the patient’s home is an act where the relational dimension is as important in the eyes of the patient – and his or her family circle – as the technical dimension of the tasks to be performed. However, in order to reconcile these two dimensions, it is essential that home care workers – whether carers or technicians – have certain information that is crucial to meeting the patient’s expectations of punctuality, efficiency and personal consideration from the first visit.
This information concerns in particular:
- How to access the person’s home – Often the address is not enough. The carers will be all the more punctual if they know where to park, what the access code is, and which floor the accommodation is on. If the patient is alone and unable to open the door, the carer needs to know where the front door key is or from which neighbour to collect it. If heavy or bulky medical equipment is to be delivered, it is equally important to know whether or not there is a lift or, if it is a house, steps to climb that would require the presence of two people.
>> All this data must be up to date, which means that it must be checked and, if necessary, updated before the visit, when the appointment is made/confirmed. It must be easily accessible and for this reason be included in the intervention sheet or in the client’s file so that it can be consulted from the carer’s mobile application. Finally, any additional information gathered in the field must be passed on to be shared with all the company’s employees likely to work with the same patient.
- The patient’s personal situation and environment – Unlike the carers, the delivery staff and technicians for HHCPs do not necessarily need to know the patient’s pathology. However, they need to know whether the planned intervention is compatible with their health condition. For example, the replacement of a conventional anti-bedsore mattress with an air mattress for an elderly person who cannot get up on his or her own can only be done in the presence of a family member or a carer who can move the patient.
>> Here again, these conditions must be checked before the visit and, if necessary, agreed with the patient’s family if we want to avoid unnecessary visits, which will have to be rescheduled in the short term anyway.
When home health professionals have all the necessary information, when their visits are properly announced, when they are assured of access to the patient’s home and of being able to carry out their tasks in conditions that are optimal for both them and the patient, they are more effective and reliable in the eyes of the patient. This is the basis of a relationship of trust, which reassures the patient and enhances the technical and relational skills of the workers.
Optimised rounds for people who really listen
If every visit to every patient is to be carried out in the best possible way, the quality of the route planning is an absolutely key aspect. This is all the more difficult because it requires more criteria to be taken into account than in any other sector due to the diversity of individual patient situations, the specific needs and constraints of each patient, and the extremely variable nature of the frequency of visits (depending on the pathologies and their evolution, the categories of care, the types of equipment, etc.)
Fortunately, planners can rely on planning and optimisation software that allows them to both:
- distribute the workload fairly among the workers according to their skills, their geographical area and the foreseeable duration of the different categories of intervention;
- easily integrate urgent visit or delivery requests, which are common in the home health sector, by offering patients pre-optimised appointment slots, i.e. taking into account the previous criteria and the appointments already scheduled;
- smoothing out predictable tasks over a long period of time, for example by automatically positioning the regulatory visits recommended by the manufacturers.
It is thus possible to draw up optimised schedules and route plans for each homecare worker, which minimise the time spent on the road and reduce the risk of delays by taking into account the distances and duration of interventions. This allows the workers to respect the schedules announced to the patients, to spend more time at their service, and to give them all the attention they have the right to expect from a health care worker.
>> Discover how Nomadia supports major healthcare and homecare providers by proposing the expertise and specialised tools they need to efficiently organise their teams, intelligently manage appointment scheduling, integrate patient constraints and, with each visit, demonstrate their ability to combine operational and relational excellence.
